Mixing medications with alcohol can lead to serious health risks, and there are 13 medications that turn dangerous when mixed with alcohol. Many people may not realize that common prescriptions and over-the-counter drugs can have harmful interactions with alcohol, which can result in side effects that range from mild to life-threatening. Understanding these risks is essential for anyone looking to stay safe and healthy.
Certain medications can cause increased drowsiness, dizziness, or even respiratory issues when combined with alcohol. Others may lose their effectiveness or create toxic reactions in the body. It is crucial to be aware of how specific medications interact with alcohol to avoid dangerous situations.
Check out these medications that should never be mixed with alcohol. Being informed can help prevent serious health complications and ensure safer choices when it comes to medication and drinking.

Acetaminophen (Tylenol)
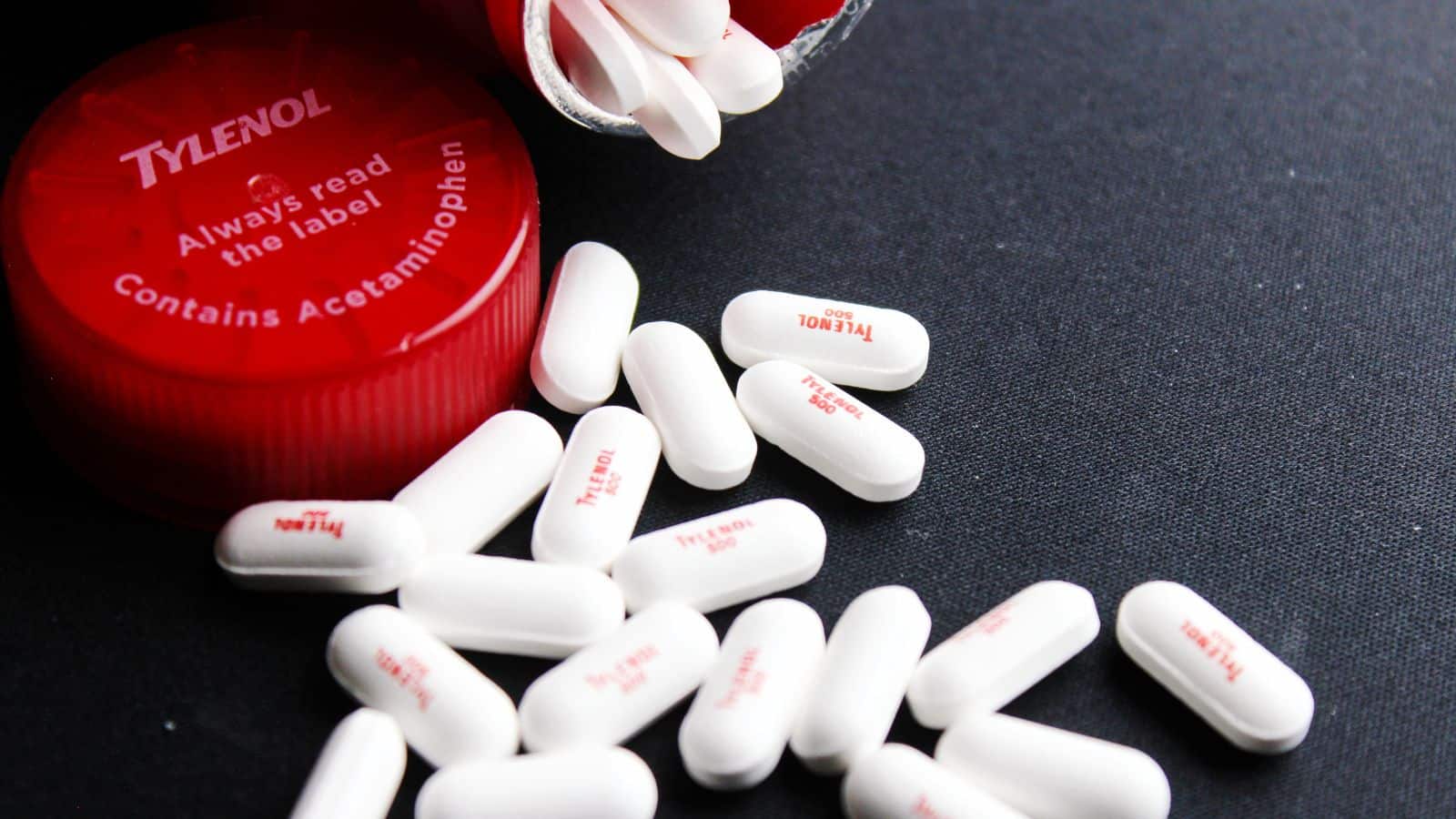
Mixing acetaminophen with alcohol can severely harm your liver, as both substances are processed by the liver. This combination increases the risk of liver failure, especially in those who consume alcohol regularly or in large amounts. The damage can be gradual, leading to cirrhosis or liver toxicity over time. When combined, alcohol can also hinder acetaminophen's effectiveness and contribute to other negative health outcomes. The combination of the two can be deadly, particularly when acetaminophen is taken in high doses, further increasing the risk of irreversible damage to vital organs, including the liver.
Benzodiazepines (e.g., Xanax, Valium, Ativan)
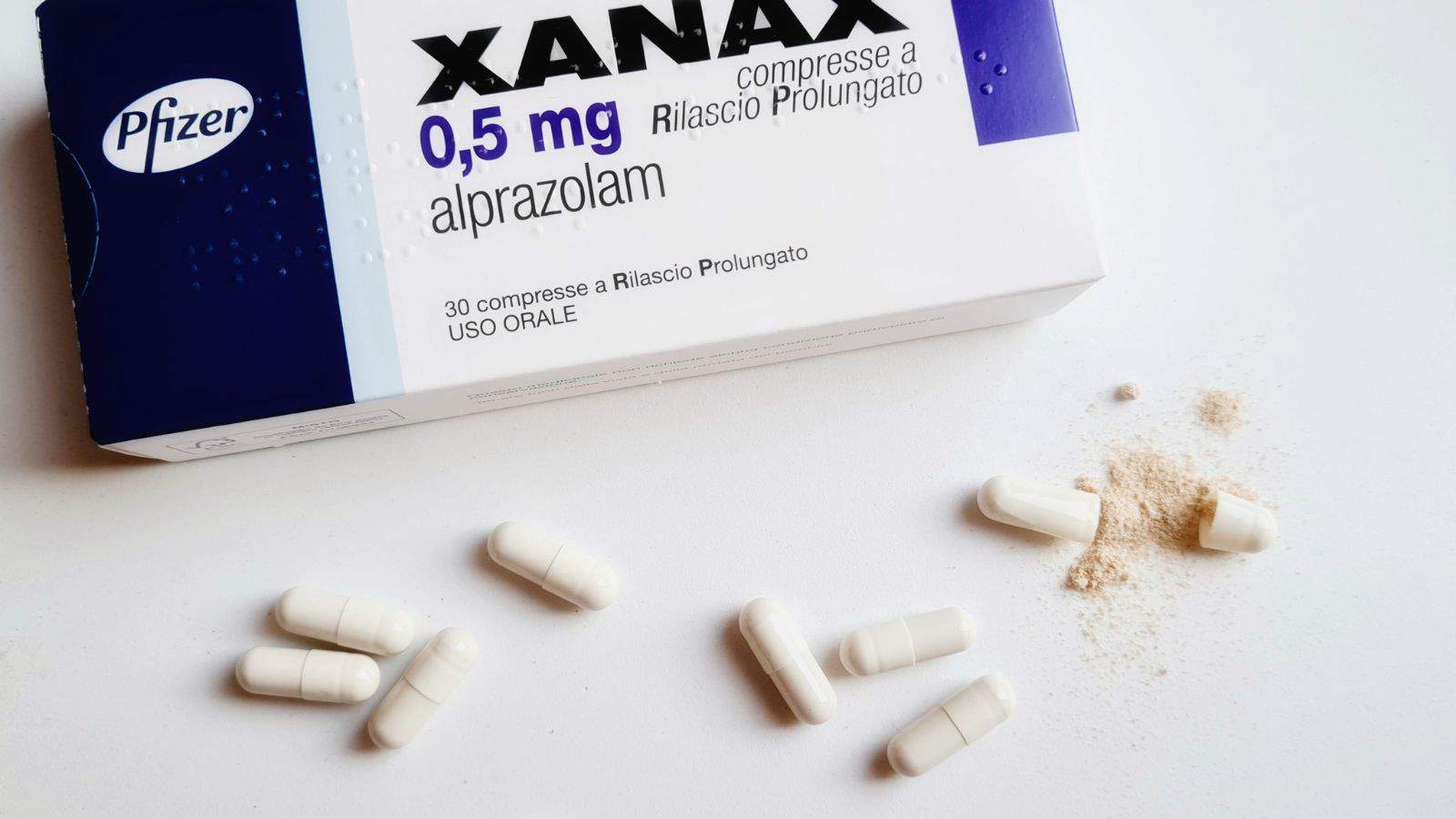
Benzodiazepines and alcohol both act as central nervous system depressants. When mixed, the sedative effects of each substance intensify, leading to severe drowsiness, dizziness, confusion, and impaired motor function. This dangerous combination can slow down breathing and heart rate, which may lead to respiratory failure, coma, or even death. Regular use of either substance or mixing them frequently can also cause dependence and increase the likelihood of overdose. These medications are often prescribed for anxiety, insomnia, and muscle relaxation, but their calming effects become risky when alcohol is involved.
Opioid Painkillers (e.g., OxyContin, Percocet)
When opioids are combined with alcohol, the depressant effects on the respiratory system become even more severe, increasing the risk of life-threatening breathing problems. Opioids already carry the risk of respiratory depression, and adding alcohol to the mix can significantly worsen this, potentially causing a fatal overdose. The combination also increases the sedative effects, leading to extreme drowsiness and confusion. Additionally, alcohol may enhance the risk of gastrointestinal issues and liver damage when the liver processes both substances. People who misuse these drugs with alcohol face an increased risk of addiction, overdose, and death.
Antidepressants (SSRIs, SNRIs)

Mixing alcohol with antidepressants, such as SSRIs or SNRIs, can increase drowsiness, dizziness, and lack of concentration, impairing mental clarity and physical coordination. For some individuals, alcohol may reduce the effectiveness of the medication, hindering its ability to manage symptoms of depression, anxiety, or other mental health disorders. More dangerously, this combination can cause serotonin syndrome, a potentially life-threatening condition marked by symptoms like agitation, confusion, rapid heart rate, and high blood pressure. Long-term mixing of alcohol and antidepressants may worsen mental health conditions, leading to negative thoughts or actions in some cases.
Antibiotics (e.g., Metronidazole, Tinidazole)

Alcohol interacts with certain antibiotics, like metronidazole and tinidazole, by causing a severe reaction that leads to symptoms like nausea, vomiting, flushing, and headaches. This is due to an interaction that prevents the breakdown of alcohol in the body, resulting in a buildup of acetaldehyde. The resulting symptoms can be highly uncomfortable and even dangerous. Alcohol can also interfere with the antibiotic's effectiveness, delaying recovery or causing the infection to persist. Mixing alcohol with antibiotics may also exacerbate side effects like dizziness or drowsiness, and in some cases, it may compromise the immune system's ability to fight infection effectively.
Antihistamines (e.g., Benadryl)
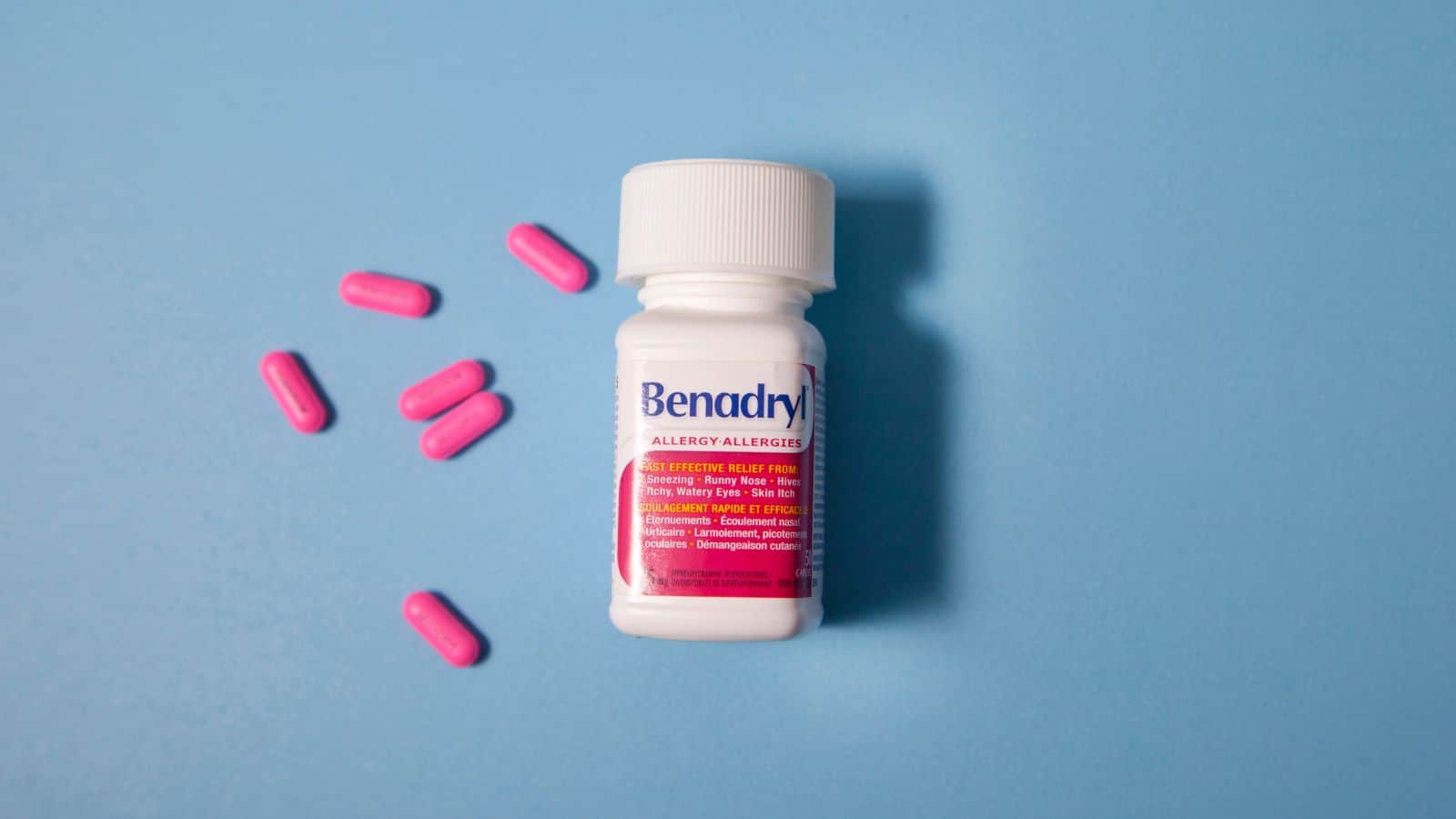
When alcohol is mixed with antihistamines like Benadryl, the sedative effects of both substances are amplified, leading to increased drowsiness and dizziness. This can impair your ability to perform daily tasks like driving, making decisions, or operating machinery. The combined depressant effects on the central nervous system can also lead to confusion and difficulty concentrating. In some cases, the mix can cause respiratory depression, which can be especially dangerous for older adults. Over time, combining these substances may increase the risk of developing chronic fatigue, and prolonged use can cause issues with memory and cognitive function.
Blood Thinners (e.g., Warfarin, Coumadin)
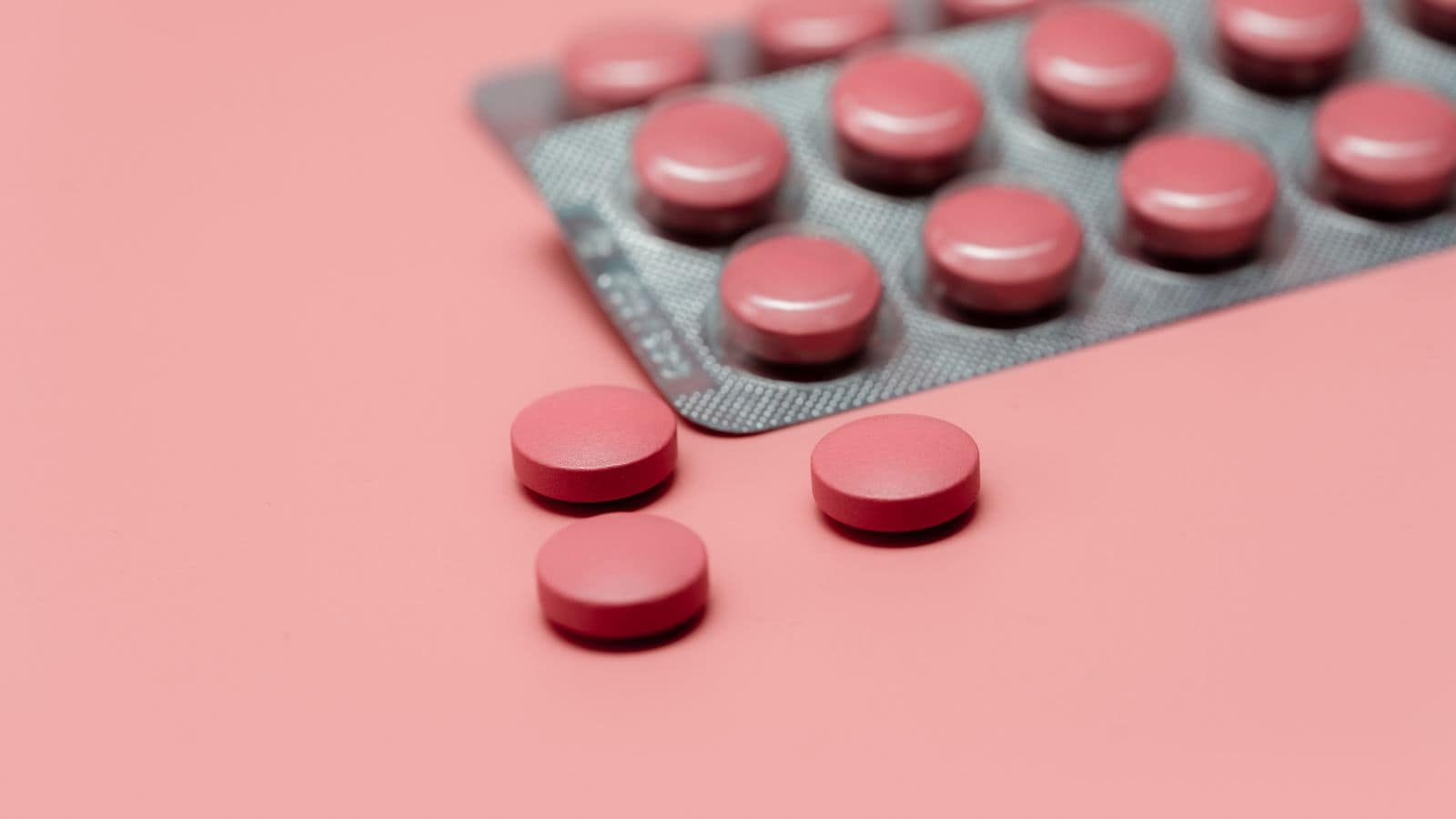
Alcohol can interact with blood thinners, such as warfarin, by altering their effectiveness and increasing the risk of bleeding. Regular alcohol consumption can cause liver damage, which impacts the liver's ability to process these medications, leading to higher or lower-than-intended blood thinning effects. This can make you more susceptible to bleeding or clotting, increasing the risk of internal bleeding, strokes, or heart attacks. Heavy drinking also heightens the risk of gastrointestinal bleeding. For those taking blood thinners, maintaining consistent alcohol consumption or avoiding alcohol altogether is crucial to preventing potentially life-threatening complications.
Anti-seizure Medications (e.g., Phenytoin, Valproate)

Alcohol can interfere with the effectiveness of anti-seizure medications, such as phenytoin and valproate, potentially increasing the likelihood of seizures. Both alcohol and these medications act on the brain, but alcohol can lower the seizure threshold, making the brain more prone to electrical disturbances. Mixing alcohol with anti-seizure medications can also cause side effects such as dizziness, drowsiness, and difficulty concentrating. Chronic alcohol use can lead to more frequent seizures and a reduction in the medication's ability to prevent them, putting the individual at greater risk for severe, uncontrolled seizures and other neurological complications.
Anti-inflammatory Drugs (e.g., Ibuprofen, Naproxen)
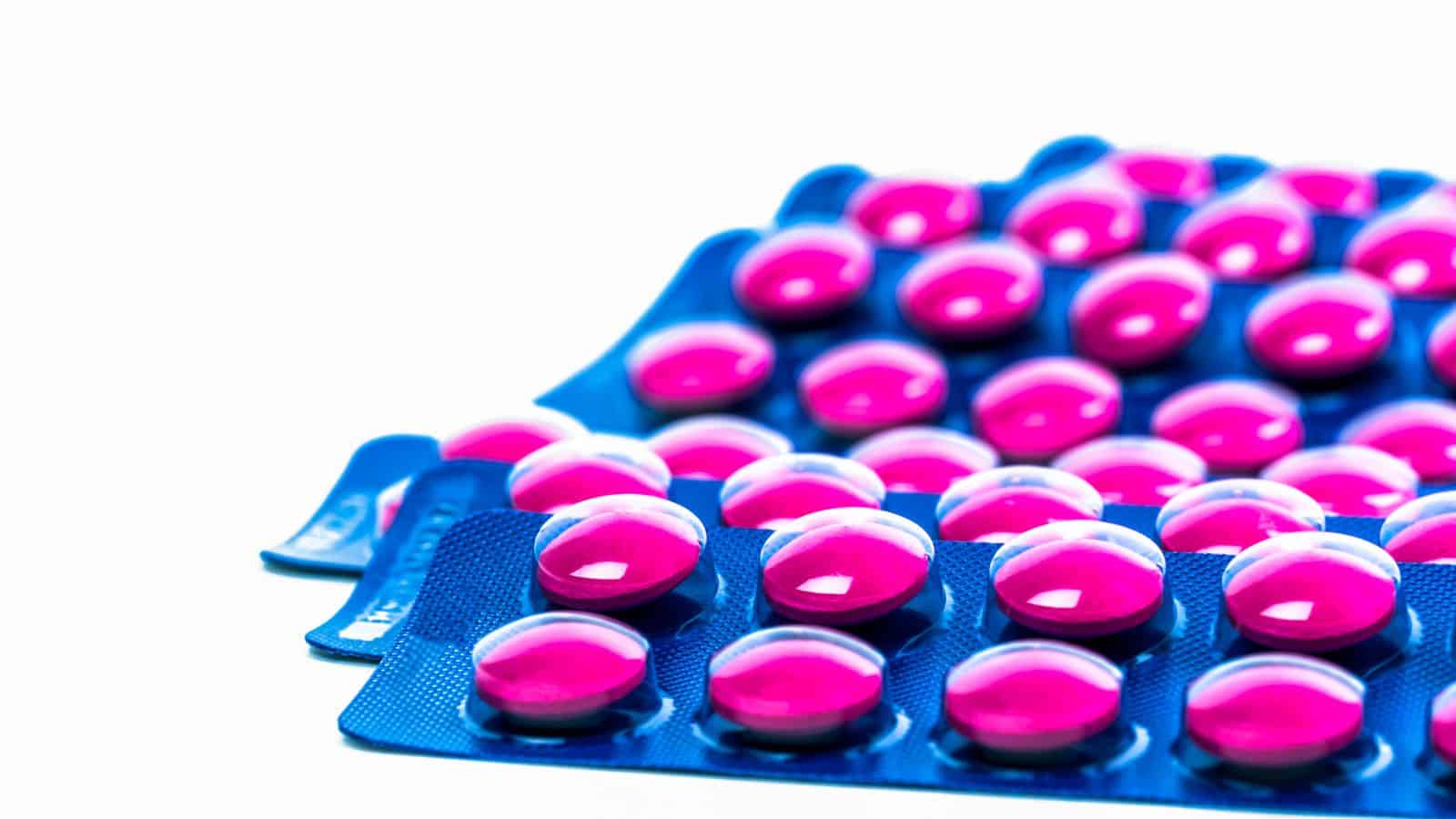
Taking alcohol with non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen increases the risk of gastrointestinal bleeding and ulcers. Alcohol irritates the stomach lining, and when combined with NSAIDs, this irritation is exacerbated, leading to potential bleeding, ulcers, or even perforations in the stomach or intestines. Both substances can also strain the liver and kidneys, and the added stress on these organs can cause long-term damage. Chronic mixing of alcohol with these medications can increase the risk of liver toxicity and kidney failure, especially in individuals with pre-existing conditions affecting these organs.
Diabetes Medications (e.g., Metformin, Insulin)

Alcohol can cause significant fluctuations in blood sugar levels when combined with diabetes medications such as metformin or insulin. This can lead to dangerously low blood sugar (hypoglycemia) or high blood sugar (hyperglycemia), both of which have serious health consequences. Alcohol can also impair the liver's ability to release glucose into the bloodstream, leading to hypoglycemia, especially if consumed without food. For those taking insulin or other diabetes medications, alcohol can increase the risk of lactic acidosis, a potentially fatal condition that causes the blood to become too acidic. Monitoring blood sugar levels closely is essential when alcohol is consumed while on these medications.
Anti-anxiety Medications (e.g., Buspirone)

When alcohol is combined with anti-anxiety medications such as buspirone, it can amplify side effects like drowsiness, dizziness, and difficulty concentrating. Alcohol may also reduce the effectiveness of the medication, making it harder to control symptoms of anxiety. This combination can impair cognitive functions, leading to challenges in decision-making and coordination. Additionally, the interaction may heighten the risk of more severe side effects, including confusion, fatigue, and mood changes. In the long term, regularly mixing alcohol with anti-anxiety medications could hinder your treatment progress and negatively affect mental well-being.
Cholesterol Medications (e.g., Statins)
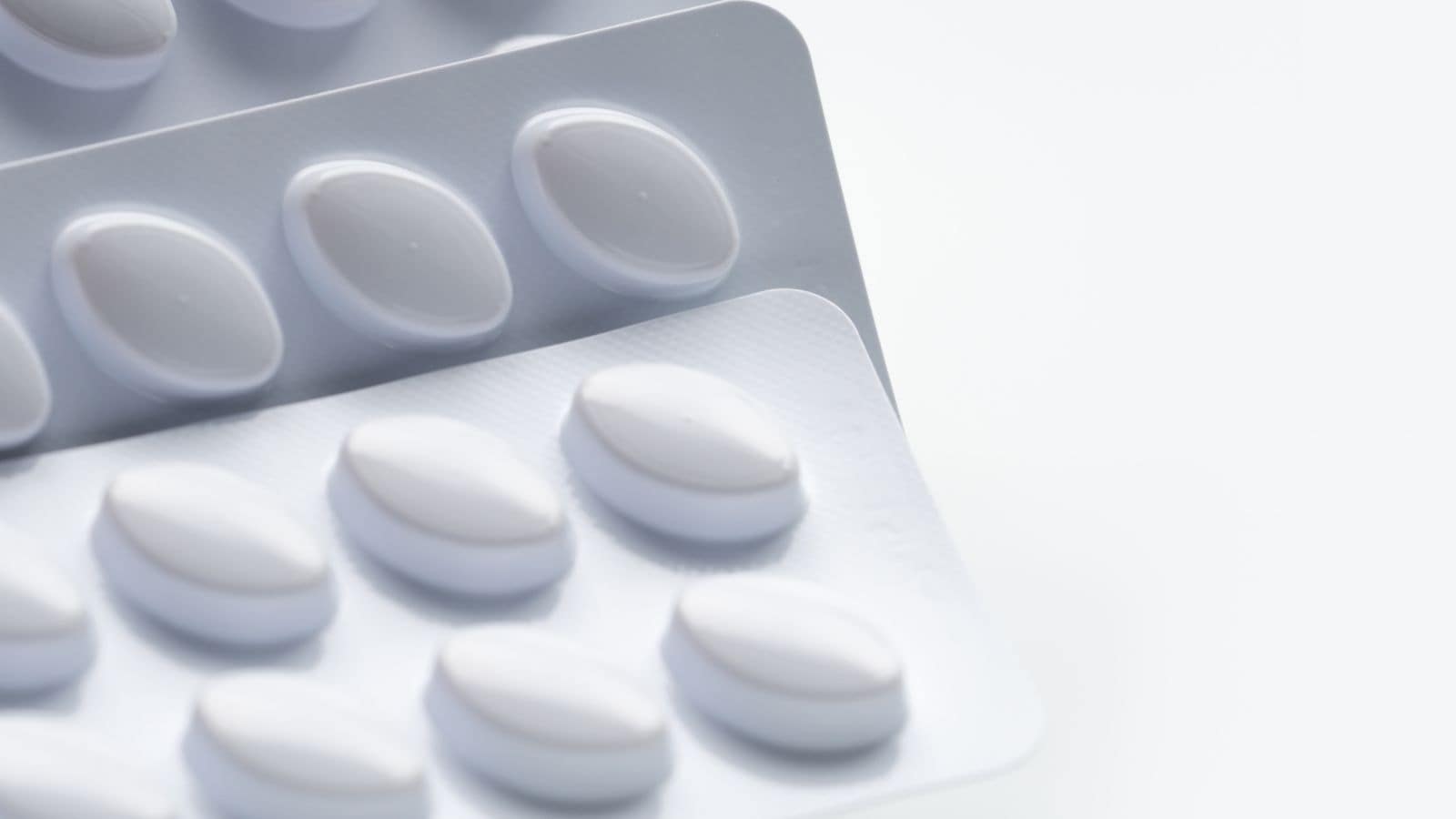
Consuming alcohol while taking cholesterol medications such as statins can increase the risk of liver damage, as both substances are processed by the liver. Alcohol can interfere with the liver's ability to metabolize statins properly, potentially increasing the levels of the medication in the bloodstream and raising the likelihood of liver toxicity. The combination can also lead to muscle pain, weakness, and even rhabdomyolysis, a rare but serious condition where muscle tissue breaks down. Long-term alcohol use may also undermine the effectiveness of statins in lowering cholesterol, which is crucial for heart health.
Sleep Medications (e.g., Ambien, Lunesta)

When alcohol is mixed with sleep medications such as Ambien or Lunesta, the sedative effects of both substances are greatly intensified, increasing the risk of extreme drowsiness, dizziness, and confusion. This can result in impaired memory and judgment, as well as difficulty coordinating movements. In more severe cases, combining alcohol with these medications can lead to respiratory depression, coma, or even death. Long-term use of both substances can also heighten the risk of developing dependency or addiction and increase the likelihood of experiencing dangerous side effects like sleepwalking or other abnormal behaviors while asleep.
9 Hidden Drinking Patterns That Worry Health Experts More Than Binge Drinking

Do you recognize a pattern? Ever think about how drinking habits can affect your life in unexpected ways? Most people know binge drinking is harmful, but there are quieter, more insidious patterns of drinking that can be just as damaging-if not worse. Unlike binge drinking, these habits don't come with obvious red flags like blackouts or severe hangovers. Instead, they creep into your daily routine, making them harder to spot.
Read More Here: 9 Hidden Drinking Patterns That Worry Health Experts More Than Binge Drinking
11 Ways to Stop a Hangover Before It Ruins Your Day

Your future self will thank you! A hangover can quickly turn a great night into a challenging day, and there are 11 ways to stop a hangover before it ruins your day. Many people underestimate the impact of what they consume and how it can affect them the next morning. Knowing how to prepare and what to do can make all the difference in feeling better and getting back to normal.
Read More Here: 11 Ways to Stop a Hangover Before It Ruins Your Day





Comments
No Comments